
 IJCP Editorial Team
IJCP Editorial Team
Sigmoidal Volvulus: A Surgical and Gynecological Challenge
Sigmoidal volvulus is a rare incidence ranging from 1 in 1500 to 1 in 66,431 deliveries. It is an intestinal obstruction in pregnancy associated with significant maternal and fetal mortality. The fundamental problem with sigmoidal volvulus is the delay in presentation and diagnosis leading to ischemia of the colon, requiring bowel resection and colostomy in most cases.
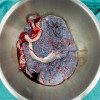
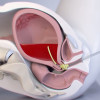
In a case, 24 weeks pregnant female, 29 years was referred from a regional hospital to Kilimanjaro Christian Medical Center with a history of 1-week abdominal pain and constipation. According to the medical history, the pain started gradually and was cramping in nature. She denied any history of fever, abdominal trauma, and vaginal discharge. She reported a decrease in fetal movement with the pregnancy being a second one after the first cesarean section. Upon examination, her blood pressure was recorded as 112/81 mmHg, pulse rate 136 beats per minute, and saturation 96% on room air. Her abdomen was symmetrically distended and moving with respiration and was tender and tense on palpation. Her blood profile was found normal but had mild hypokalemia, which was corrected by intravenous potassium chloride. Abdominal X-ray suggested intestinal obstruction with a differential perforated hollow viscus. Following the diagnosis, she consented to an emergency laparotomy, and after the operation and following the postoperative period, she was found clinically stable with no complaints of pain or any other issues.
The classical presentation of sigmoidal volvulus is abdominal distension, constipation (30%), abdominal pain (98%), and vomiting (82%) which can be unspecified in pregnancy as they can be related to pregnancy. Also, clinical examination is limited due to the gravis uterus, and radiological evaluation presents another detrimental effect leading to the teratogenicity of the fetus. Sigmoidal volvulus in pregnancy requires a multidisciplinary approach including obstetric and pediatric teams. Before laparotomy, resuscitation is vital with decompression, fluids, and correcting electrolytes is needed. Endoscopy can be another examination method with a success rate of up to 50-80% in non-pregnancy states.
Source: Lodhia, J. et al., J Med Case
Reports 15, 554 (2021).
https://doi.org/10.1186/s13256-021-03151-3

IJCP Editorial Team
Comprising seasoned professionals and experts from the medical field, the IJCP editorial team is dedicated to delivering timely and accurate content and thriving to provide attention-grabbing information for the readers. What sets them apart are their diverse expertise, spanning academia, research, and clinical practice, and their dedication to upholding the highest standards of quality and integrity. With a wealth of experience and a commitment to excellence, the IJCP editorial team strives to provide valuable perspectives, the latest trends, and in-depth analyses across various medical domains, all in a way that keeps you interested and engaged.
















Please login to comment on this article