Childhood obesity has become a major global public health concern, affecting children across both developed and developing countries. While some weight gain is a normal part of growth and development, excessive weight gain can lead to serious health complications that extend into adulthood.
What Do the Statistics Say?
|
Childhood obesity is a rapidly growing
global health crisis, with the number of affected children and adolescents
rising sharply over the past three decades.
India is experiencing
a similarly concerning trend.
· Under-five obesity
rose by 127% and currently, nearly 33 million children in the country are
living with overweight or obesity.
· By 2030, India is
projected to contribute 11% of the global childhood obesity burden, with the
affected population expected to surge to 83 million by 2035.
|

Fig 1: Global Prevalence of Obesity in Children
|
What Is Childhood Obesity?
Childhood
obesity is a complex, long-term medical condition that occurs when a child’s
weight is higher than what is considered healthy for their age, height, and
sex. For children aged 2 years and older, obesity is medically defined as
having a Body Mass Index (BMI) at or above the 95th percentile for age and sex.
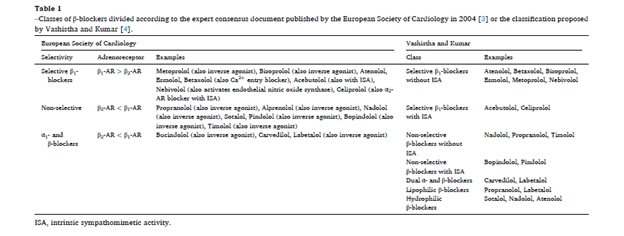
Fig 2: Depicts the BMI based weight categorization in Children
What Causes Childhood Obesity?
There is no single cause of childhood obesity. It results from a combination of genetic, environmental, and lifestyle factors.
1. Poor Nutrition: Diets high in processed foods, added sugars, and unhealthy fats contribute significantly to weight gain. Increased portion sizes and easy access to inexpensive junk food further worsen the problem.
2. Lack of Physical Activity: Many children spend more time watching television, playing video games, or using mobile devices than engaging in active play.
3. Family Habits: Children tend to adopt the eating and activity patterns of their families. When healthy behaviors are modeled at home, children are more likely to follow them.
4. Socioeconomic Challenges: Limited access to affordable healthy foods and safe play areas can make it difficult for families to maintain healthy lifestyles.
5. Medical and Genetic Factors: Certain health conditions, medications, and genetic predispositions can also contribute to weight gain.
In addition, societal factors such as aggressive marketing of unhealthy foods, reduced physical education in schools, and unsafe outdoor environments further complicate prevention efforts.
Why Is Childhood Obesity Dangerous?
Childhood obesity affects much more than appearance. It increases the risk of serious health conditions, including:
|
- Depression
and low self-esteem
|
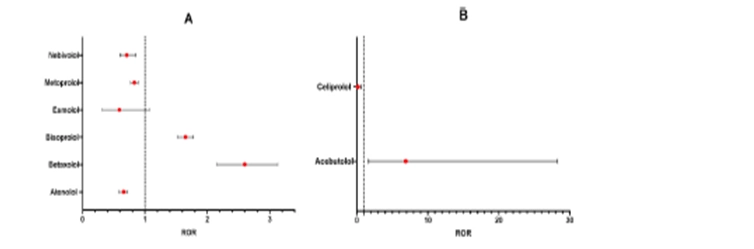
Fig 3: Health Risks of Childhood Obesity
|
Children with obesity are also more likely to become adults with obesity, increasing their long-term risk of chronic disease.
How Can Childhood Obesity Be Prevented?
There is no quick fix. Preventing childhood obesity requires consistent, balanced efforts from families, schools, communities, and healthcare systems. Here are practical steps parents can take:
1. Encourage Healthy Eating Habits
• Prioritize fruits, vegetables, whole grains, lean proteins, and healthy fats
• Limit processed foods and sugary drinks
• Serve balanced meals with appropriate portion sizes
• Encourage children to listen to hunger and fullness cues
• Avoid using food as a reward or punishment
Breastfeeding exclusively for the first six months may also reduce obesity risk later in life.
2. Promote Daily Physical Activity
Children should get at least 60 minutes of physical activity per day. This doesn’t require structured workouts. Encourage:
• Outdoor play
• Cycling or walking
• Team sports
• Dancing or family activities
• Active commuting to school where possible
Reducing screen time to less than 1–2 hours per day can significantly improve activity levels.
3. Foster a Positive Relationship With Food and Exercise
Focus on overall health rather than weight alone. Avoid negative language about body size. Emphasize strength, energy, and well-being instead. Parents play a powerful role by modeling healthy behaviors — cooking at home, staying active, and maintaining balanced routines.
4. Support Emotional Well-Being
Stress, anxiety, depression, and sleep deprivation can contribute to unhealthy eating patterns. Healthy minds support healthy bodies. Parents can:
• Encourage open conversations about emotions
• Teach stress-management techniques
• Watch for signs of bullying or social isolation
5. Set Simple Routines for Better Sleep
|
Adequate
sleep is a powerful yet often overlooked pillar of a child’s health. Sleep
needs vary by age.
·
Preschoolers
require 10–13 hours
of sleep per day (including naps).
·
Children
aged 6–12 years need 9–12
hours of uninterrupted sleep each night,
·
Teenagers
aged 13–17 years should aim for 8–10
hours nightly.
|
|

Fig
4: Depicts benefits of adequate sleep
|
Establishing simple routines such as fixed bedtimes and wake-up times, even on weekends can significantly improve sleep quality. Creating a calm bedtime environment and limiting screen time before bed further supports healthy sleep habits that protect long-term health.
6. Replace Screen Time with Family Time
Reducing screen time creates valuable opportunities for family interaction whether it’s sharing meals, playing outdoors, reading together, or simply talking about the day. Simple steps can make a meaningful difference.
• Turn off screens at least one hour before bedtime and keep electronic devices out of children’s bedrooms.
• Establishing clear, consistent family media rules to create a balanced routine that supports both physical and emotional well-being.
7. Schedule Regular Pediatric Checkups
Routine visits allow healthcare providers to monitor growth patterns and identify potential concerns early. Pediatricians can offer guidance on nutrition, activity, and overall health.
8. Adapt Strategies to Your Family’s Reality
Prevention should be realistic and sustainable. Cultural traditions, economic factors, and local resources all influence lifestyle choices. Small, consistent changes are more effective than drastic restrictions.
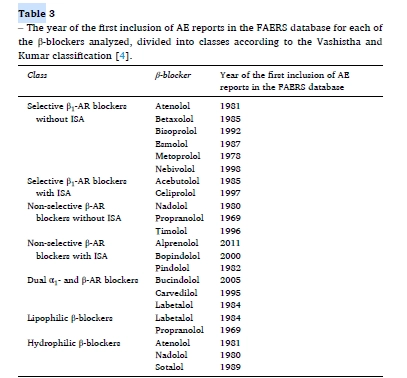
Fig: 5 The Long-Term
Benefits of Obesity Prevention
Conclusion
Preventing childhood obesity requires a supportive and informed approach. It is not about strict dieting or focusing solely on weight. Instead, it is about nurturing balanced nutrition, regular physical activity, emotional resilience, and healthy routines from an early age.
When families focus on overall wellness rather than numbers on a scale, children are more likely to thrive physically, emotionally, and socially.
References:
1. World Health Organization. Obesity and overweight. WHO; 2024 [cited 2026 Feb 12]. Available from: https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight
2. UNICEF India. India: Overweight and obesity rising across all ages – from youngest children to adults. UNICEF; [cited 2026 Feb 12]. Available from: https://www.unicef.org/india/press-releases/india-overweight-and-obesity-rising-across-all-ages-youngest-children-adults#:~:text=According%20to%20the%20National%20Family,CNNS%202016%2D18
3. Centers for Disease Control and Prevention (CDC). Family and obesity. CDC; 2023 [cited 2026 Feb 12]. Available from: https://www.cdc.gov/obesity/family-action/index.html
4. Veldhuizen S, Wormgoor MEA. Childhood obesity: prevalence, consequences and prevention. Front Pediatr. 2022;10:8801824. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8801824/
5. Barlow SE, Dietz WH. Obesity evaluation and treatment: Expert committee recommendations. J Pediatr Health Care. 2004;18(6):305–31. Available from: https://www.jpedhc.org/article/S0891-5245(04)00275-5/fulltext
6. Johns Hopkins Medicine. Preventing obesity. Johns Hopkins Medicine; [cited 2026 Feb 12]. Available from: https://www.hopkinsmedicine.org/health/conditions-and-diseases/obesity/preventing-obesity
7. Cleveland Clinic. Obesity in children. Cleveland Clinic; [cited 2026 Feb 12]. Available from: https://my.clevelandclinic.org/health/diseases/9467-obesity-in-children
8. Buonomo E, Miozzo M, et al. Epidemiology and determinants of childhood obesity: A comprehensive review. Front Nutr. 2023;10:10089268. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10089268/
9. Mayo Clinic Staff. Childhood obesity: Diagnosis and treatment. Mayo Clinic; 2024 [cited 2026 Feb 12]. Available from: https://www.mayoclinic.org/diseases-conditions/childhood-obesity/diagnosis-treatment/drc-20354833
10. Mountain Family Health Centers. Childhood obesity prevention: A supportive guide for parents. MountainFamily.org; [cited 2026 Feb 12]. Available from: https://mountainfamily.org/news/childhood-obesity-prevention-a-supportive-guide-for-parents/














Please login to comment on this article