
 IJCP Editorial Team
IJCP Editorial Team
Rare Advanced Abdominal Pregnancy with Severe Preeclampsia
A report describes a case of a 24-year-old unbooked primigravida who was 40 weeks post-date and had a spontaneous conception. She presented symptoms and signs of severe preeclampsia, an episode of diffuse abdominal pain, recurrent vaginal spotting, nausea, and loss of appetite for two days.
Physical examination revealed her blood pressure as 190/110 mmHg, pulse rate as 94 beats/minute, temperature as 37˚C, respiratory rate as 20 minutes, and oxygen saturation (SPO2) as 97% on room air. She was awake and alert, in pain and anxious but not in distress or cyanotic. Her skin and mucous membranes were pale.
Her respiratory and cardiovascular examinations were normal. Abdominal examination revealed an enlarged abdomen, soft on palpation, moderately tender, and without protective muscle tension. Palpation showed the parts of the fetus's body in the transverse position. Auscultation revealed a positive fetal heartbeat of 150 beats/minute. She showed no clear border of the uterus nor any signs of uterine contraction.
Pelvic examination revealed a closed, posterior, and unaffected cervix. The patient showed hyperreflexia but no focal neurological deficits and no signs of free fluid in the abdominal cavity.
She was admitted to the intensive care unit for stabilization, managing elevated B.P. with magnesium sulfate and labetalol, and planned for an emergency cesarean section (C.S.). The initial investigations revealed 7.1 g/dl of Hb and normal liver, renal, and coagulation profiles. Her urinary protein by catheter was +3.
An urgent ultrasound revealed a single intra-abdominal viable pregnancy with a gestational age of 37+, an empty uterus, fluid inside the cul-de-sac, and an expected fetal weight (EFW) of 2.8 kg and a biophysical profile (BPP) of 6/8 with decreased liquor. Doppler showed vascularization of the uterine fundus. She didn't show any tissues between the anterior abdominal wall and parts of the fetus. However, Doppler revealed a formation of 12 × 10 cm in the right uterine appendage area with intense blood flow. She showed no signs of amniotic fluid but described a small amount of peritoneal fluid in the left pericolic pocket.
She received a diagnosis of progressive abdominal pregnancy.
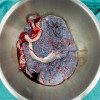
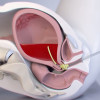
Intraoperatively, she showed an empty uterus, with the placenta adherent to the bowel and the presence of about 4 liters of blood. Moreover, after separating the adhesion, she showed a defect in the right cornu. She underwent small bowel adhesiolysis and repairing of the small serosa tear. She delivered a live male fetus (weighing 2.6 kg, with an Apgar score between 7 and 9 points and no major birth defects) stained with meconium from the abdominal cavity during the operation.
Since admission, the patient received six units of PRBC, six units of platelets, three units of fresh frozen plasma, and one unit of cryoprecipitate. She also received ceftriaxone and metronidazole for five days.
The patient got discharged from the hospital with her baby in good general health. She received a regular follow-up. Her blood β-HCG was restored to normal levels three weeks following surgery. She remains under close monitoring and is experiencing no pain.
Musalli F, Atef G, Al-Attas A. Successful Management of Rare Advanced Abdominal Pregnancy with Severe Preeclampsia: A Case Report and Literature Review. Open Journal of Obstetrics and Gynecology. 2022;12: 907-913. doi: 10.4236/ojog.2022.129075.

IJCP Editorial Team
Comprising seasoned professionals and experts from the medical field, the IJCP editorial team is dedicated to delivering timely and accurate content and thriving to provide attention-grabbing information for the readers. What sets them apart are their diverse expertise, spanning academia, research, and clinical practice, and their dedication to upholding the highest standards of quality and integrity. With a wealth of experience and a commitment to excellence, the IJCP editorial team strives to provide valuable perspectives, the latest trends, and in-depth analyses across various medical domains, all in a way that keeps you interested and engaged.
















Please login to comment on this article