
 IJCP Editorial Team
IJCP Editorial Team
Portal Cavernoma in Pregnancy
A report describes the case of a 32-year-old, gravida 3 para 2, pregnant woman. She had a history of hospitalization at 11 weeks of gestation due to back pain and fever, where she was diagnosed with pyelonephritis and given antibiotic therapy with endovenous cefalexin. Her complaints were resolved in a few hours. However, a routine abdomen scan displayed a solid, hyperechoic material inside a swollen portal vein. The portal vein had increased calibre with numerous channels. Doppler imaging confirmed the diagnosis of PVT and she was referred to a tertiary hospital at 13 weeks and 1 day of gestation.
On admission, she was clinically asymptomatic, without signs of hypersplenism or portal cholangiopathy. She was hemodynamically stable. Transabdominal ultrasound showed a single fetus with a CRL of 67 mm, confirming 13 weeks of gestation. Screening for Down's syndrome showed a low-risk. The nuchal translucency was found to be 1.3 mm, nasal bone was evident, and no signs of tricuspid regurgitation and normal wave-a on the ductus venosus were seen.
The previous history revealed a gastric sleeve procedure last year for third-degree obesity. She did not have a history of liver disease.
Laboratory investigations showed a mild normochromic normocytic anemia and a moderately high level of transaminases. Platelets count, prothrombin time, partial thromboplastin time and bleeding time were normal. The thrombotic risk profile came out to be negative for major deficiencies.
Viral and/or autoimmune hepatitis tests were also negative. The abdominal examination displayed a nontender, non-distended abdomen, without pain and with normal bowel sounds. Mild splenomegaly with no signs of ascites was recorded.
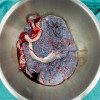
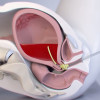
Abdominal ultrasound showed hepatomegaly (right lobe hypertrophy) with nonhomogeneous hepatic echostructure and portal vein thrombosis with cavernomatous transformation. Inflammatory abdominal foci or free ascitic fluid within the abdominal cavity were absent. The cavernomatous transformation of the portal venous system in the hilar region of the liver extending to the intrahepatic system was confirmed by Color Doppler US.
An upper digestive endoscopy ruled out esophageal varices.
She was administered subcutaneous low-molecular-weight heparins of 16.000 units, for treating venous thromboembolism. The activated partial thromboplastin time (PTT) and the platelet count tests were performed weekly to rule out heparin-induced thrombocytopenia and to review liver and renal functions.
Her pyelonephritis resolved in a few days. She explained all the maternal and fetal risks about the possibility of developing esophageal varices and/or other collateral circulation, ascites, and hypersplenism. Termination of pregnancy as per the guidelines was offered and performed with consent.
Savoia F, Ferrara C, Sansone A, Bifulco G, Nappi C, Di Carlo C. Portal Cavernoma during Pregnancy. Case Rep Obstet Gynecol. 2013;2013:396083. doi:10.1155/2013/396083

IJCP Editorial Team
Comprising seasoned professionals and experts from the medical field, the IJCP editorial team is dedicated to delivering timely and accurate content and thriving to provide attention-grabbing information for the readers. What sets them apart are their diverse expertise, spanning academia, research, and clinical practice, and their dedication to upholding the highest standards of quality and integrity. With a wealth of experience and a commitment to excellence, the IJCP editorial team strives to provide valuable perspectives, the latest trends, and in-depth analyses across various medical domains, all in a way that keeps you interested and engaged.
















Please login to comment on this article