 IJCP Editorial Team
IJCP Editorial Team
Pediatric Fulminant Cerebellitis
An otherwise healthy 12-year-old male presented with severe headache over the past two months. The headaches seemed progressive and were associated with fever. The child reported severe headache with nausea and vomiting on the day of hospitalization.
There was no history of photophobia or neck stiffness. On examination, the child did not elicit an abnormal eye movement or gait. The vital signs were stable.
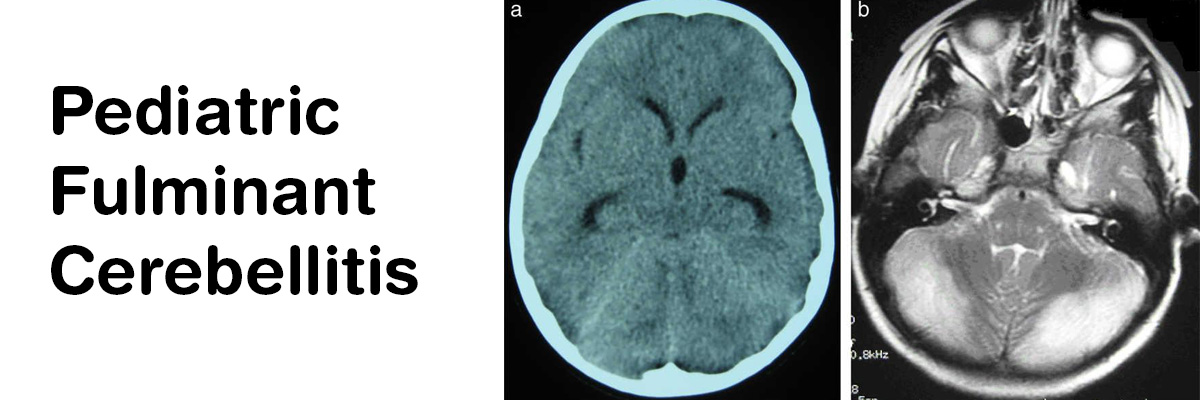
Computed tomography (CT) scan imaging revealed obstructive hydrocephalus along with diffuse cerebellar swelling compressing the fourth ventricle. The cerebellar tonsils were slightly depressed.
Neurosurgery was planned for cerebrospinal fluid (CSF) diversion with the insertion of a ventriculoperitoneal (VP) shunt, based on the diagnosis of acute hydrocephalus precipitated due to acute post-infectious cerebellitis.
The follow-up magnetic resonance imaging (MRI) 24 hours after the VP shunt insertion depicted regression of the hydrocephalus. The patient was prescribed acyclovir 20 mg/kg/dose TID, vancomycin 20 mg/kg/dose QID, and ceftriaxone 50 mg/kg/dose BID.
However, all blood/CSF cultures revealed negative results. Thereafter, pulse steroid therapy 30 mg/kg daily for 3 days was prescribed, along with intravenous immunoglobulin (IVIG) 1 gm/kg for 2 days, for treating the fulminant cerebellitis.
This led to clear clinical and radiological improvement. A follow-up MRI confirmed resolution and normalization of cerebellar structures. There were no major sequelae at the three-month checkup.
Source: The American Journal of Case Reports. 2021 Jan 17;22:e928370. doi: 10.12659/AJCR.928370.

IJCP Editorial Team
Comprising seasoned professionals and experts from the medical field, the IJCP editorial team is dedicated to delivering timely and accurate content and thriving to provide attention-grabbing information for the readers. What sets them apart are their diverse expertise, spanning academia, research, and clinical practice, and their dedication to upholding the highest standards of quality and integrity. With a wealth of experience and a commitment to excellence, the IJCP editorial team strives to provide valuable perspectives, the latest trends, and in-depth analyses across various medical domains, all in a way that keeps you interested and engaged.















Please login to comment on this article