
Published On: 29 Aug, 2025 11:41 AM | Updated On: 29 Aug, 2025 11:53 AM
Necrotic Vaginal Pressure Ulcer with Introitus Collapse: Surgical Repair Using Vulvar Flaps
Presentation
A teenage paraplegic patient presented with a 1-month history of persistent
vaginal discharge, initially treated as presumed candidiasis. On examination,
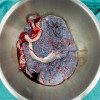
extensive necrotic eschar was identified involving the posterior fourchette,
vestibule, and vaginal tissue extending to the pubic bone, with sparing of the
labia majora. CT imaging excluded necrotizing fasciitis. Prompt debridement of
necrotic tissue and initiation of broad-spectrum antibiotics were undertaken.
Operative Findings
and Repair
Coordinated intervention by pediatric and adolescent gynecology and plastic
surgery revealed an open circumferential vestibular wound. The inferior labia
minora and urethral meatus were absent, the vaginal introitus had collapsed at
the wound base, and a 3 × 4 cm segment of the retropubic ligament was exposed.
The distal mucosal edge was separated from underlying tissue.
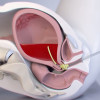
Reconstruction included:
- Advancement of the
posterior vaginal wall to reconstitute the introitus.
- Overlapping
transposition of large vulvar flaps to resurface anterior and lateral
defects, covering the retropubic ligament.
- Fasciocutaneous
advancement flaps with wide subfascial undermining to achieve vulvar
closure.
- Placement of an
estrogen-coated soft vaginal stent to maintain patency.
Outcome
The combined surgical approach successfully restored vaginal and vulvar anatomy
and preserved functional capacity despite extensive tissue loss.
Conclusion
This case underscores the critical importance of early recognition, aggressive
debridement, antimicrobial therapy, and coordinated surgical reconstruction in
managing severe vulvovaginal necrosis in complex patients.













Please login to comment on this article