
 IJCP Editorial Team
IJCP Editorial Team
Hypertriglyceridemia with Acute Pancreatitis in Pediatric Diabetic Ketoacidosis: A Case Report
Diabetic Ketoacidosis (DKA) is one of the commonest diagnoses observed in the Pediatric Intensive Care Unit (PICU). It is associated with fatal complications like cerebral edema, however non-fatal complications like hypertriglyceridemia and pancreatitis can also be encountered but are very rare.
A case reports a previously healthy, non-obese, 16-year-old African-American female who complained of difficulty in breathing. Two weeks before, she was diagnosed with oral thrush and prescribed nystatin by her primary care physician. She also gave a history of polyuria, polydipsia, weight loss, and decreased energy for a few days before the presentation.
The local community hospital diagnosed DKA (serum glucose > 500 mg/dL, urine glucose > 1000 mg/dL, urine ketone > 80 mg/dL, capillary blood pH of 6.8, and serum sodium 110 mEq/L).
Since she had moderate-to-severe dehydration, was given two litres (~30 ml/kg) of crystalloid fluid bolus; and also received an intravenous (IV) insulin bolus and sodium bicarbonate bolus before getting transferred to a tertiary care center.
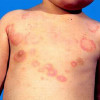
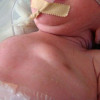
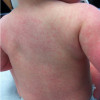
After admitting to PICU, she continued to show severe metabolic acidosis. Her examination indicated Kussmaul's breathing, altered mental status reacting only to painful stimuli, and signs of poor perfusion (tachycardia up to 140/min, capillary refill time of 3-4 seconds, and bilateral weak peripheral pulses). She also showed skin lesions described as multiple yellowish firm papules, around both knees and scattered over the face and trunk. Point-of-care serum sodium level was found to be 122 mEq/dL but the laboratory tests were not performed on the sample since it was "too thick". A blood sample from the peripheral IV line was difficult to obtain and once obtained, it had chances to turn "milky".
Her serum sodium displayed a downward trend despite improvement in her metabolic acidosis. Hyperlipidemia was suspected based on the appearance of her blood sample. Her serum triglyceride (TG) level was recorded to be 930 mg/dL and total cholesterol 332 mg/dL.
Continuous IV insulin drip and twice maintenance IV fluids were given to her. She showed improvement in her mental status eight to ten hours after the admission and stabilization of serum glucose but developed diffused abdominal pain with anorexia 12 hours following admission to PICU. Lab investigations revealed serum amylase to be 155 unit/L and lipase to be 1100 unit/L. Abdominal ultrasound revealed acute pancreatitis and ruled out acute appendicitis, gall stone, and pancreatic pseudocyst. Between 12 to 36 hours following admission, her highest serum TG level was 2515 mg/dL, her highest serum amylase was 612 unit/L, and highest serum lipase was 5387 unit/L.
Pancreatitis and lack of appetite directed continuation of insulin drip and maintenance of IV fluid even after resolution of her metabolic acidosis. Serum glucose was measured every two hours, with no record of any hypoglycemic episode.
Her appetite improved along with the downward trend of serum TG (614 mg/dL) and serum lipase (574 unit/L), nearly 48 hours after admission. She was initiated fenofibrate for hyperlipidemia, consulted with the dermatologist for skin lesions, and confirmed xanthoma by pathology report.
SOURCE= Yagnik PJ, Desai PH, Modem VM. Hypertriglyceridemia with Acute Pancreatitis in Pediatric Diabetic Ketoacidosis: A Case Report. Cureus. 2019;11(1):e3844. Published 2019 Jan 8. doi:10.7759/cureus.3844

IJCP Editorial Team
Comprising seasoned professionals and experts from the medical field, the IJCP editorial team is dedicated to delivering timely and accurate content and thriving to provide attention-grabbing information for the readers. What sets them apart are their diverse expertise, spanning academia, research, and clinical practice, and their dedication to upholding the highest standards of quality and integrity. With a wealth of experience and a commitment to excellence, the IJCP editorial team strives to provide valuable perspectives, the latest trends, and in-depth analyses across various medical domains, all in a way that keeps you interested and engaged.















Please login to comment on this article