 IJCP Editorial Team
IJCP Editorial Team
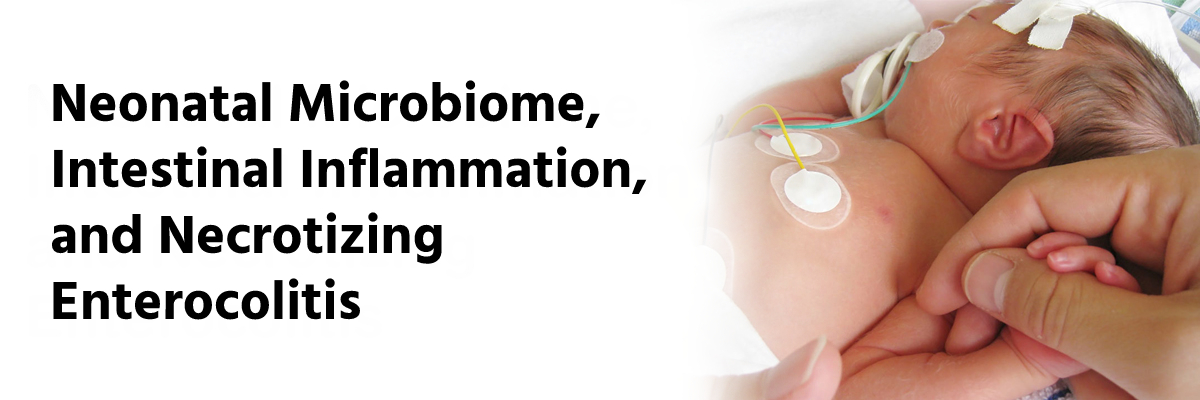
Neonatal Microbiome, Intestinal Inflammation, and Necrotizing Enterocolitis
Necrotizing enterocolitis (NEC) is the most common gastrointestinal emergency in the neonatal intensive care unit (NICU). It is also a major cause of preterm infant morbidity and mortality. Along with others, its driving factors include intestinal barrier immaturity, hyperinflammatory immune cells, and dysbiosis. Intestinal inflammation, frequently after enteral feeds, results in bacterial translocation of the intestinal barrier, sepsis, multiorgan failure, and sometimes death.
NEC pathophysiology remains incompletely understood even years after research progress, and treatment options are limited to surgical and supportive therapies. Infants surviving this devastating disease frequently suffer from neurodevelopmental impairment, short gut syndrome, intestinal failure, and cerebral palsy.
Recently, animal modeling in germ-free or Toll-like receptor knockout (TLR KO) mice has suggested dysbiosis' probable role in driving NEC pathogenesis. Numerous factors, modifiable and unmodifiable, affect gut microbiome development in preterm infants, including infant gestational age, mode of delivery and feeding, infant medications, and maternal and NICU environment.
- Burge KY and Markel TA, in a Special Issue published in Microorganisms, describe:
- Recent developments in the understanding of preterm infant gut microbiome development and progression;
- Methods to noninvasively detect shifts in microbiome composition for use as biomarkers;
- Promising developments in the use of prebiotics, probiotics, or synbiotics for preventing or ameliorating severe intestinal inflammation in premature infants.
Infant Gut Microbiota:
The collective intestinal microbiome assumably determines NEC pathogenesis. Unlike healthy term infants, the microbiome of preterm infants has distinct but less diverse taxa, with a progression dictated largely by postmenstrual age. Components of these host-microbe interactions cause the basal tuning of the preterm immune system to luminal contents, breakdown of the intestinal barrier, and resulting runaway intestinal epithelial inflammation characteristic of NEC.
Microbiome Detection and Identification of Biomarkers:
Volatile organic compounds (VOCs) are the recently described noninvasive fecal biomarkers of microbiome shifts that diagnose NEC even before the appearance of obvious symptoms; and can be detected via gas chromatography (GC), mass spectrometry (MS), and, very recently, electronic nose (eNose) technology. There is limited use of eNose technology in clinical applications due to non-standardized protocols for stool acquisition and differences in signals among age groups and dietary patterns. Further, elevated DL-lactate and a reduction in enzymes capable of utilizing human milk oligosaccharides (HMOs) may also emerge as the potential biomarkers of developing preterm dysbiosis and NEC.
Prebiotics, Probiotics, and Synbiotics:
Prebiotics, probiotics, and synbiotics continue to draw interest for prevention or therapeutic use in NEC because, when used in the early postnatal period, they are capable of modulating preterm infant microbiome development, thus potentially mitigating or preventing the development of NEC.
Burge KY, Markel TA. Neonatal Microbiome, Intestinal Inflammation, and Necrotizing Enterocolitis. Microorganisms. 2022 Jul 9;10(7):1382. DOI: 10.3390/microorganisms10071382. PMID: 35889101; PMCID: PMC9320150.

IJCP Editorial Team
Comprising seasoned professionals and experts from the medical field, the IJCP editorial team is dedicated to delivering timely and accurate content and thriving to provide attention-grabbing information for the readers. What sets them apart are their diverse expertise, spanning academia, research, and clinical practice, and their dedication to upholding the highest standards of quality and integrity. With a wealth of experience and a commitment to excellence, the IJCP editorial team strives to provide valuable perspectives, the latest trends, and in-depth analyses across various medical domains, all in a way that keeps you interested and engaged.













Please login to comment on this article